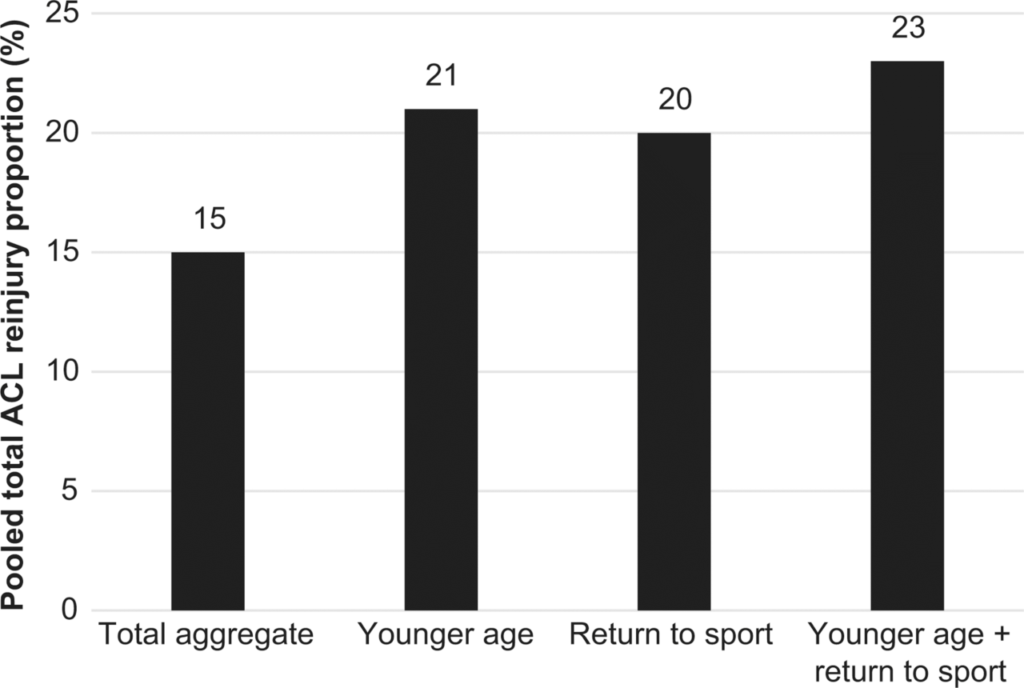Physical Therapist
Background:
Anterior cruciate ligament (ACL) rupture rate is the highest in young athletes who participate in sports involving cutting and pivoting (basketball, skiing, soccer) and when they occur tend to be season-ending injuries requiring surgical reconstruction. Female sex and young age have been viewed as common risk factors for initial injury. Even after successful surgical reconstruction and rehabilitation, reinjury to the reconstructed ACL and/or ACL of the opposite limb can occur. At this time, research suggests that environmental and genetic factors may be causes of reinjury. Recently, more studies have become available focusing on the rates of reinjury in younger active individuals, but their results have not been summarized.
Literature search and data analysis to determine possible risk factors for reinjury:
In a recent article by Wiggins et al researchers reviewed existing literature and analyzed data found within to evaluate whether a patient’s age and activity level could be seen as risk factors for another ACL injury following reconstruction.
The researchers narrowed down a database search to 19 articles for review. Then they recorded data from populations included in these articles regarding: total ACL reinjury rate (of the same side and/or opposite limb), specific sport an individual returned to if provided, the nature of the sport (low risk or high-risk involving cutting/jumping), and demographics.
The researchers hypothesized that returning to sport and a younger age would place individuals at higher risk for a second ACL injury.
An analysis was performed on the data from the entire included population and a separate analysis was performed on data sets broken down by individuals of a young age, those who returned to a sport, and from those who were young and returned to a sport.
Results
- In individuals across all ages who underwent ACL reconstruction: 7% reinjured the same ACL and 8% reinjured the opposite side
- In individuals < 25 years old who underwent ACL reconstruction: 21% had another ACL injury with 11% being the opposite knee
- In individuals who returned to sports following reconstruction: 20% had another ACL injury with 12% being the opposite knee
- In individuals who were <25 years old who returned to high-risk sport following reconstruction: 23% had another injury with 12%
Conclusion
Individuals who return to a high-risk sport and those of a younger age are at risk for ACL reinjury. Almost one-fourth of individuals who are of a younger age (<20-25) and return to a high risk sport that involves pivoting and cutting will either reinjure the reconstructed ACL or injure the opposite side. Based on the current literature the majority of these secondary injuries occur in the knee that has not undergone previous surgical intervention.
What Can Physical Therapists Do to Prevent Reinjury?
Individuals who have or have not undergone a previous ACL repair can be examined by a physical therapist who can determine if they are at risk for injury/reinjury due to factors such as:
- The individual’s improper performance of functional movements
- Muscular imbalances
- Strength and flexibility deficits
- Improper running and landing mechanics
- Balance deficits
- Asymmetrical strength/power between limbs
Your therapist will then address these issues with a personalized plan of care which may include but is not limited to interventions such as:
- Exercises to strengthen or improve flexibility in specific muscles
- Plyometric or jump training
- Activity modification recommendations
- Neuromuscular re-education
- Bracing
Original Article: Wiggins Amelia, Grandhi Ravi, Schneider Daniel, Stanfield Denver, Webster Kate, Myer Gregory. Risk of secondary injury in younger athletes after anterior cruciate ligament reconstruction: A systematic review and meta-analysis Am J. Sports Med. 2016 July; 44(&): 1861-1876